Lung Function Centre
A lung function test is a series of breathing tests where you will be required to breathe in different patterns through a mouthpiece. These patterns may require you to breath fast, inhale big breaths, exhale until your lungs are empty and hold your breath. The respiratory scientist conducting the test will talk you through each process. A lung function test is a simple, non-invasive way to examine your lungs and your breathing.
What sort of problems are diagnosed by these tests?
There are many different reasons your doctor may request you get a lung function test. Some of these reasons include:
- To diagnose the cause of a cough or shortness of breath
- Possible diagnoses of Asthma, Chronic Obstructive Bronchitis, Emphysema, Lung Fibrosis, Asbestosis.
- To evaluate the severity of disease
- To see if you are fit to undergo major surgery
- As a general check-up for lung health, especially if you have had exposure to cigarette smoke or other hazardous chemicals
- To track disease progression
What do I need to bring to my test?
If you use any inhalers bring these along with you to your test. Wear comfortable clothes that will not restrict your breathing
How long will the test take?
The lung function test generally takes about 30 minutes. The exact length of the test will vary for each individual.
Could I feel unwell during the test?
During the testing you may feel a little bit breathless. The tests can also make you cough and you may feel lightheaded for a few seconds. This is normal and you will be given time to recover between tests. There are no side-effects from testing and you will be able to drive home afterwards.
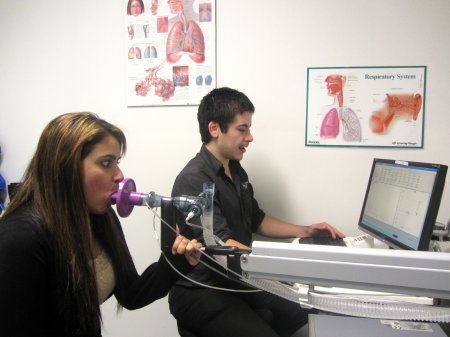
How are the tests done?
The Scientist will spend time with you to explain the process; it involves having you blow into a machine which measures the amount of air you can exhale and how fast you can expel the air from your lungs. It also measures whether your breathing has improved after inhaling a ‘bronchodilator’ puffer (e.g. Ventolin). In some cases, additional testing may establish how well the lung membranes are working. This indicates how well oxygen can pass from the lungs across the membranes into your blood stream. In the case of diagnosing asthma, a ‘bronchial challenge test’ will be performed to see how sensitive your airways are to inhalation of very low doses of a drug which may identify if there is likely to be an asthma tendency.
Are the tests painful?
No. The tests do require that you are making your best effort to ensure the most accurate results are
available to your doctor. Part of the training undertaken by the Respiratory Scientist is to ensure that you are comfortable throughout the procedure, but performing to the best of your ability.
Do I have to withhold taking any medications on the day or day before the tests?
Yes. The following medication should be withheld for the specified hours before the test. If it is necessary for relief, you may use your usual reliever, but please advise staff prior to the test.
Specific test instructions:
For Spirometry, Gas exchange, Nitrogen and Muscle Strength Test, please note the following:
| Medication | Hours to withhold prior to test |
| Reliever: Ventolin, Bricanyl, Atrovent, Asmol, Airomir, etc | 8 |
| Symbicort, Alvesco, Seretide, Pulmicort, Flixotide, Oxis or Foradil | 12 |
| Spiriva, Singulair, Tilade | 24 |
| Antihistamine tablets: Clarityne, Hismanal, etc | 48 |
All patients are asked to refrain from the following before all tests:
| Activity | Hours to withhold prior to test |
| Smoking | 3 |
| Consuming alcohol or caffeinated drinks | 4 |
| Performing vigorous exercise | 1 |
| Eating a large meal | 2 |
| Wearing restrictive clothing |
Bronchial Challenge Test
The Mannitol/Aridol challenge test requires some small preparation for the results to be interpreted accurately.
You have been asked by your doctor to perform a Bronchial Challenge Test. During the test you will inhale some Aridol – which is a sugary powder. Between doses you will perform spirometry (a simple breathing test) to assess how your lungs respond to the Aridol. It is important that you do not take certain medications prior to your test – please refer to the following table. If you feel you need to take your medications do not hesitate to take them, and call your doctor to reschedule your test appointment.
| Medication | Hours to withhold prior to test |
| Caffeine (coffee, energy drinks, cola or chocolate), do not smoke or perform vigorous exercise. | Day of test |
| Reliever: Ventolin, Bricanyl, Atrovent, Asmol, Airomir, Intal, Tilade | 8 |
| Symbicort, Alvesco, Seretide, Pulmicort, Flixotide, Oxis, Qvar, Becloforte, Becodite or Foradil | 12 |
| Spiriva, Singulair, Tilade | 24 |
| Antihistamine tablets: Clarityne, Hismanal, Telfast, Zyrtec, etc | 48 |
MEDICAL PRACTITIONER TECHNICAL INFORMATION
It is staffed by our Sleep and Respiratory Scientists. They are trained in Respiratory Laboratory Technology
requiring the blended skills of interacting with patients to ensure that the best performance is achieved in the tests and operating the respiratory function equipment to provide the most useful information for the referring practitioner.
Respiratory function tests are invaluable in identifying possible causes of breathlessness, asthma, COPD, and the numerous interstitial lung diseases.
The main tests undertaken by the laboratory are:
1.Spirometry and Flow Volume Loops
These tests involve the measurement of lung volumes before and after bronchodilator. The reported results include Forced Vital Capacity (FVC), Forced Expiratory Volume in 1 sec (FEV1), FEV1/FVC%, Peak Flow, and Flow volume profiles to identify evidence of small airways disease, including flow rates at 50% Vital Capacity (V50). The tests are repeated until reproducible results are obtained. The Laboratory Scientist will report on the adequacy of the patient’s performance on technical grounds. Predicted values are reported, based on the age and height of the patient. Although weight is not factor in determining predicted results, it is recognized as a factor in contributing to a restrictive defect (reduced FVC), and to aid in this interpretation we provide a calculation of Body Mass Index (BMI). The tests allow the identification of airflow obstruction, restriction, and responsiveness to bronchodilator. The request form contains information regarding withholding medication prior to the tests to ensure that responsiveness can be evaluated.
2. Gas Diffusion (DLCO)
This is a complex test that evaluates the diffusing capacity for carbon monoxide, to determine how effectively oxygen can diffuse from the alveolar space across the alveoli and into red blood cells. The test is carried out by asking the patient to breathe right out, then to take a rapid breath in to the maximum breathing in a gas mixture containing a low concentration of CO and methane, holding the breath for 10seconds and then expiring rapidly to close to residual volume. The results of the volume inspired, time of breath hold and 4 gas concentrations are required to compute the diffusing capacity. It measures more than the membrane diffusion, so that other factors may have an influence on the results obtained, including anaemia, polycythemia, intrapulmonary haemorrhage, recent high intensity exercise, thyroid disease, and smoking just before the test. The result of a recent Haemoglobin is requested as we can then provide an adjusted result for an ‘idealised Hb’. Patients are advised to refrain from smoking for 3 hours before the test, to reduce the confounding effects of CO in cigarette smoke. Causes of a low diffusing capacity include emphysema, interstitial lung disease, asbestosis, anaemia, hypothyroidism, cardiac failure and pulmonary hypertension. It is expected to be normal in an asthmatic who has never smoked. A poor technical performance- eg doing a Valsalva manoeuvre during the 10sec breath-hold may cause a low result. The Scientist will be watching for this.
A high diffusing capacity may be seen in polycythemia, and intrapulmonary haemorrhage.
3. Bronchial Provocation Tests
This follows from the spirometry test, and requires the patient to have an acceptable FEV/FVC ratio before commencement for safety reasons. Incremental doses of the provocative agent are administered, until there is a fall in FEV1 of 15% from the baseline, or the dose protocol is completed.
A 15% fall is taken as a positive result. This would support the diagnosis of asthma, but there are other reasons for a false positive, including a recent URTI- within the past 6 weeks, allergic rhinitis, or taking beta-blockers. False negative results are uncommon. It would be most unusual for an asthmatic to have a negative result. The use of inhaled corticosteroids may attenuate the level of bronchial hyper-reactivity
The value of the test is either in supporting the clinical diagnosis of asthma, seeking an explanation for chronic cough or in excluding asthma.
4. Nitrogen Wash-out Test
A nitrogen washout can be performed with a single nitrogen breath, or multiple ones. Both tests use similar tools, both can estimate functional residual capacity and the degree of non uniformity of gas distribution in the lungs, but the multiple-breath test more accurately measures absolute lung volumes. The following describes a single-breath nitrogen test:
A subject takes a breath of 100% oxygen and exhales through a one-way valve measuring nitrogen content and volume. A plot of the nitrogen concentration (as a % of total gas) vs. expired volume is obtained by increasing the nitrogen concentration from zero to the percentage of nitrogen in the alveoli. The nitrogen concentration is initially zero because the subject is exhaling the dead space oxygen they just breathed in (does not participate in alveolar exchange), and climbs as alveolar air mixes with the dead space air. The dead space can be determined from this curve by drawing a vertical line down the curve such that the areas below the curve (left of the line) and above the curve (right of the line) area equal.
Most people with a normal distribution of airways resistances will reduce their expired end-tidal nitrogen concentrations to less than 2.5% within seven minutes. Individuals with high resistance in their airways can take longer than seven minutes to remove all the nitrogen.
5. Respiratory Muscle Strength Test
Respiratory muscle strength can be assessed by measuring the maximal inspiratory pressure (MIP, PImax, or negative inspiratory force [NIF]) and the maximal expiratory pressure (MEP or PEmax). The MIP reflects the strength of the diaphragm and other inspiratory muscles, while the MEP reflects the strength of the abdominal muscles and other expiratory muscles. Common indications for measurement of the MIP and MEP include:
- Respiratory muscle weakness is suspected, such as a patient with dyspnoea, weak cough, and known neuromuscular disease.
- Spirometry detected a pattern of restriction: reduced forced expiratory volume in one second (FEV1), reduced forced vital capacity (FVC), normal FEV1/FVC ratio, and reduced total lung capacity (TLC) and respiratory muscle weakness is in the differential diagnosis.
- Spirometry detected a low vital capacity (VC) of unknown etiology and respiratory muscle weakness is in the differential diagnosis.
- Spirometry detected a low maximal voluntary ventilation (MVV) maneuver of unknown etiology and respiratory muscle weakness is in the differential diagnosis.
- Evaluation of whether known respiratory muscle weakness has improved, remained stable, or worsened.
- To determine whether there is an increased risk of incident mobility disability in older individuals, hospitalizations and death in patients with COPD, mortality in patients with heart failure.